Higher Thinking
Quick, timely blog posts. Thought-provoking trends. How-to guides and in-depth case studies. Use this page to explore all of our best thinking on US healthcare delivery, plus the occasional news from our firm. Find something that inspires or troubles you? Contact us any time – we’d love to be your thought partner in delivering more accessible, sustainable, and equitable healthcare. >>
Blog Posts

April 16, 2024
When Will PE Give Up on Physician Practices?
New research suggests that PE firms don't know how to make money on physician practices. Here's what that means for provider planning.
Blog Posts

March 26, 2024
Meet the Team: Kim Meymandi
How an illness led this senior consultant into a healthcare career – with a special focus on improving access for underserved communities.
Blog Posts

March 7, 2024
Healthcare Workforce Development: Learning from Bloomberg
Student debt is a big hurdle to healthcare workforce development, but Bloomberg Philanthropies is betting that it doesn't have to be.
Case Studies

February 13, 2024
Securing the Future of a County-Owned Hospital
Here’s how we helped elected leaders in one rural county secure a brighter future for the county-owned hospital.
Blog Posts
January 22, 2024
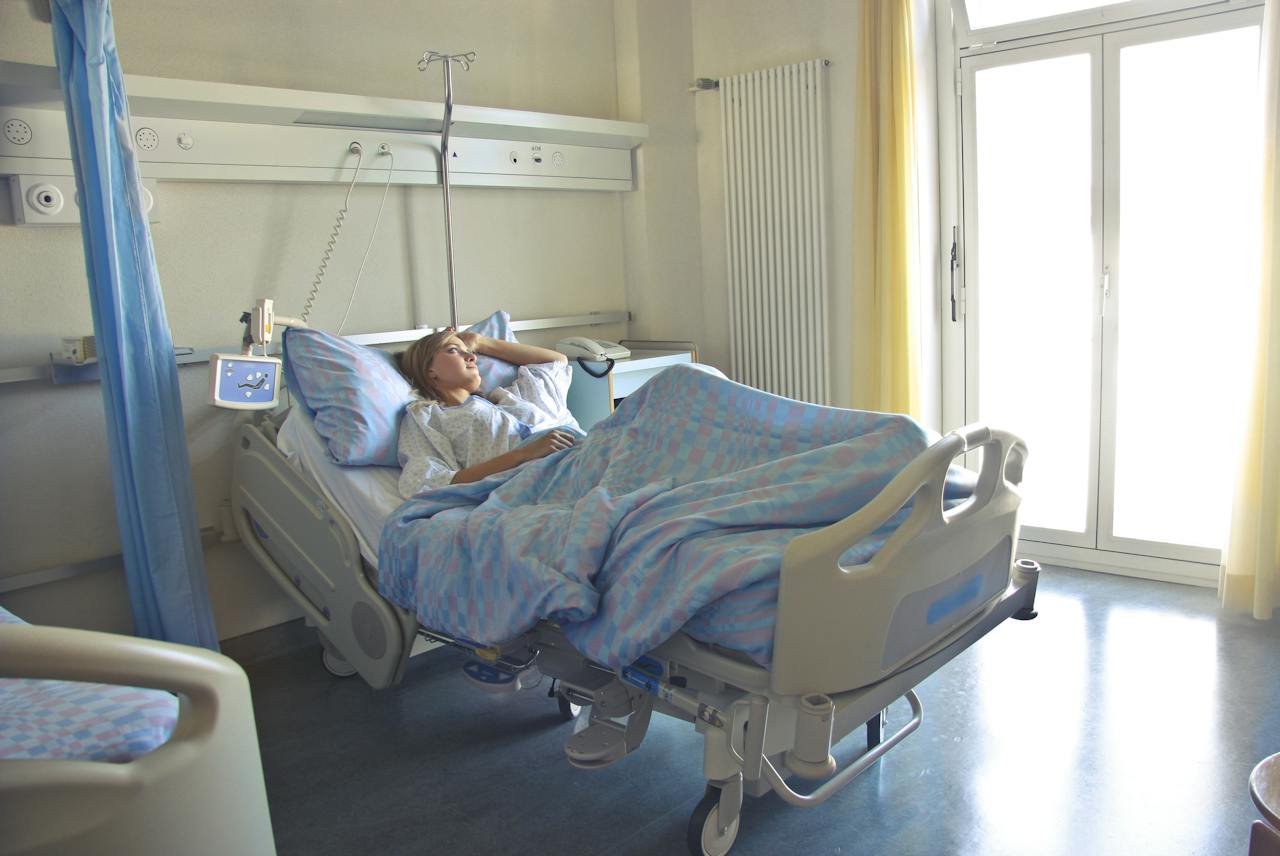
Medicare (Dis)Advantage: Hospital Observation Downgrades
Research shows that observation status is much more common under Medicare Advantage – bad news for patients and hospitals alike.
Blog Posts

January 11, 2024
Hospital Operating Margins in Limbo as Investments Drive Profitability
Hospital operating margins are highly uncertain, even as investment income provides an illusion of financial wellbeing.
Blog Posts

January 4, 2024
Meet the Team: Patricia Dowbiggin
Our strategy consultant discusses her background in EMS, her burden for rural healthcare ... and her love of the outdoors.
Firm News

December 19, 2023
Celebrating Another Year of Impact
Here's what happened when our far-flung team gathered in NC for a 2023 holiday party.
Blog Posts

December 18, 2023
Medicare (Dis)Advantage: DRG Downgrades
MA plans are using millions of DRG downgrades as a "backdoor" tool for cutting hospital payments. Here are 3 ways to fight back.
Blog Posts

November 21, 2023
Medicare (Dis)Advantage: 35 Million Prior Authorizations
Prior authorizations have become the norm in Medicare Advantage, causing treatment delays for patients and financial headaches for providers.
Blog Posts

November 16, 2023
Medicare (Dis)Advantage: Hospitals Count the Cost
Medicare Advantage now covers more than half of U.S. seniors, putting huge new strains on healthcare delivery.
Blog Posts

November 7, 2023
Total Cost of Care: Lessons from the Maryland Model
A Maryland expert shares her experience with total cost of care as CMS pushes other states to consider the approach.
Blog Posts

October 31, 2023
Why Private Equity Is No Strategy for Struggling Hospitals
For providers in imminent danger of closing their doors and stopping all service, private equity might be better than nothing. But only just.
Blog Posts
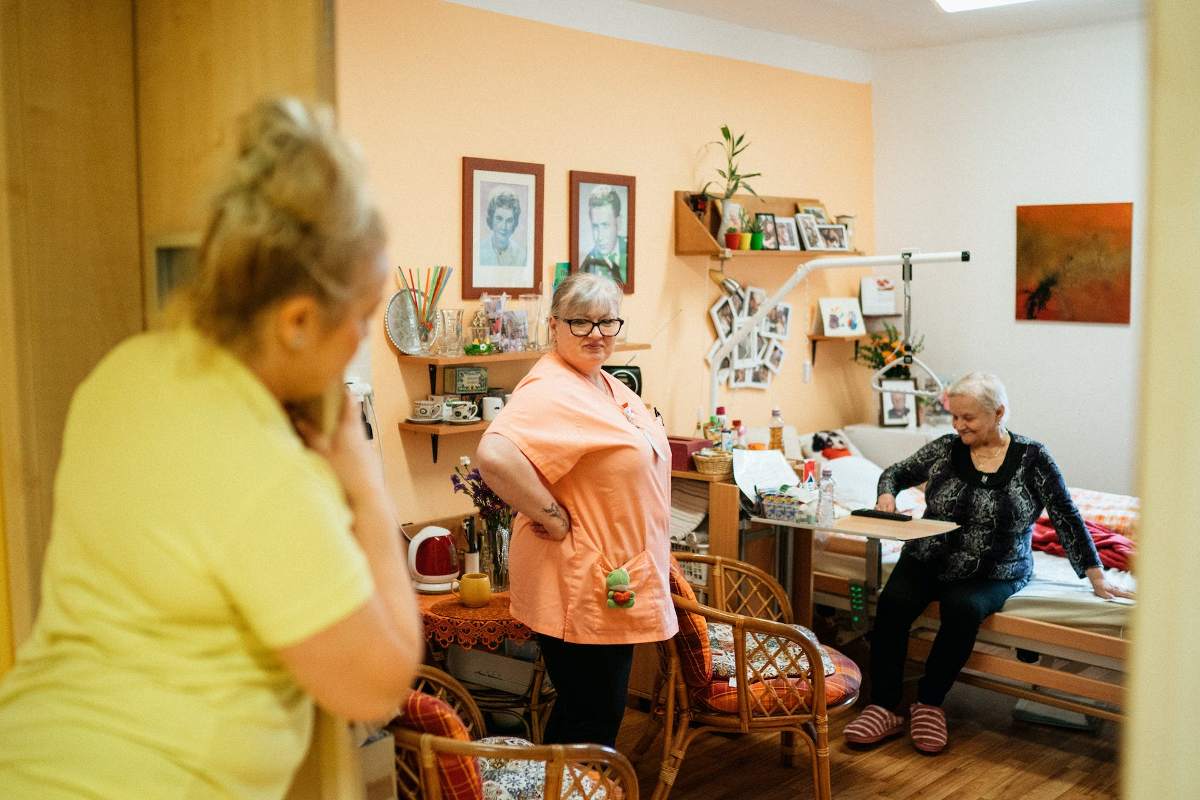
October 26, 2023
Why the Post-Acute Crisis Is Acutely Troubling for Hospitals
Nursing homes are facing unprecedented staffing challenges in 2023 – with big implications for hospitals.
Firm News

October 18, 2023
Ascendient Aids County After Hospital Closure (Video)
When a rural hospital was closed unexpectedly, Ascendient stepped in to find a more sustainable option for local healthcare.
Blog Posts

October 11, 2023
Can a New CMS Model Move Healthcare Transformation AHEAD?
Thoughts on the newest CMS model, based on our deep expertise with Maryland's TCOC model.
Guides

October 10, 2023
Ascendient’s Guide to the Maryland Model and the Path AHEAD
Maryland's experiment with Total Cost of Care offers a glimpse of the future for states considering the new AHEAD model from CMS.
Guides

September 14, 2023
Public Health Strategic Planning: the Ascendient Guide
Where are we? Who are we? Where are we going? Those three questions are the key to public health strategic planning in a time of turmoil.
Firm News

September 12, 2023
Introducing the New Healthcare Research e-Brief from Ascendient
Each month, the Ascendient Research Team curates and analyzes the most pressing, most actionable healthcare research.
Firm News

September 6, 2023
Meet the Team: Greg Flicek
Our resident CPA discusses where he came from, what drives him, and what he'd like to fix in healthcare.